How to Choose Zirconia Blocks: From Single Crowns to Full-Arch Restorations Guide
2025-12-29
2026-03-21
In North American dental practices, complete dentures remain one of the most common yet labor-intensive restorations. For decades, heat-cured polymethyl methacrylate (PMMA) has been the gold standard. Today, 3D printed photopolymer resins are disrupting this space, offering faster production, fewer patient visits, and predictable outcomes. With the US digital denture market projected to grow from USD 516 million in 2025 to USD 806 million by 2031 at a 6.5% CAGR, and North America holding a dominant 37.3% share of the global digital denture sector, clinics that adopt digital workflows gain a clear competitive edge.
This article delivers a practical, data-driven roadmap for North American clinics transitioning from conventional heat-cured PMMA to 3D printed resin dentures—without hype, just real metrics and actionable steps.
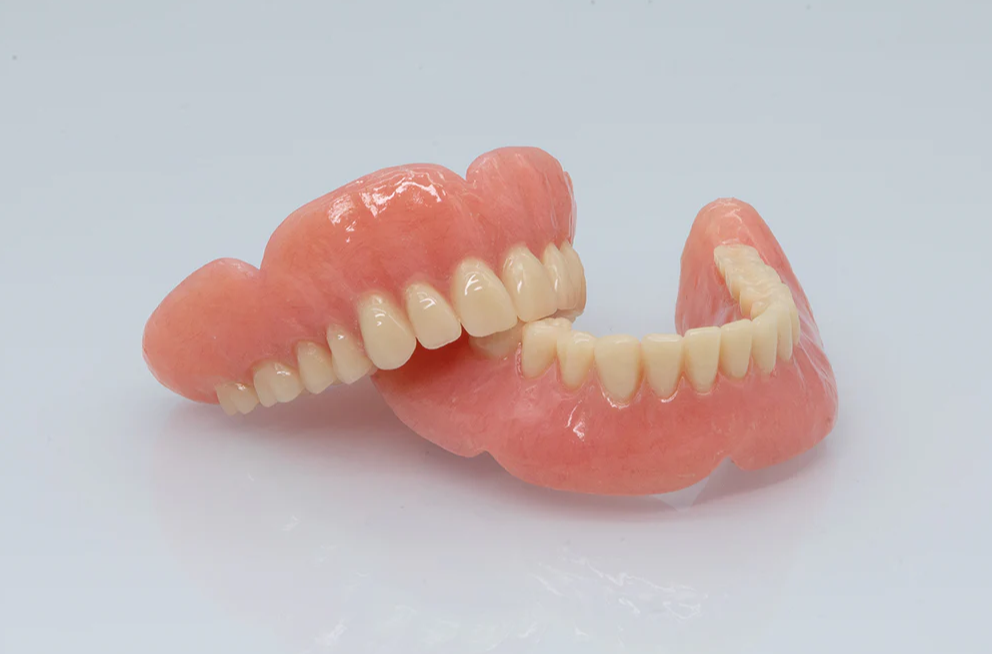
Traditional Heat-Cured PMMA Heat-cured PMMA dentures are fabricated using a flasking, packing, and long thermal polymerization process (typically 74–100°C for 8–12 hours, plus bench cooling). The material offers proven flexural strength (often >80 MPa), excellent impact resistance, and strong tooth-to-base bonding. However, the analog workflow involves multiple pourings, wax setups, and manual finishing—prone to polymerization shrinkage (0.5–2%), distortion, and human error. Production takes 2–6 weeks, requiring 5+ clinical appointments.
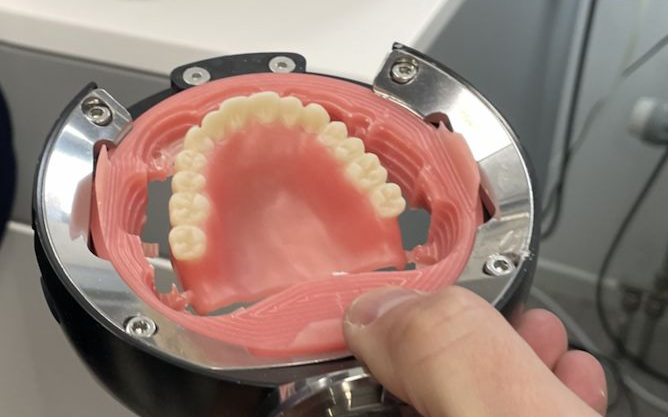
3D Printed Resin (Photopolymer Liquid) Digital dentures start with intraoral or lab scans, CAD design, and additive manufacturing via vat polymerization. Liquid resin is cured layer-by-layer (typically 50–100 µm layers) under UV light, followed by post-curing. Key advantages include minimal material waste, high dimensional accuracy (often <50 µm deviation), and production in 24–48 hours. While early resins showed lower flexural strength than PMMA, optimized printing orientations (e.g., 90° vertical) and extended post-curing (≥30 minutes) now deliver comparable or superior mechanical performance in select studies, with lower water sorption in controlled conditions.
| Aspect | Traditional Heat-Cured PMMA | 3D Printed Resin Dentures | Winner for Clinics |
|---|---|---|---|
| Production Time | 2–6 weeks | 24–48 hours | 3D Printed |
| Clinical Appointments | 5–6 visits | 2–4 visits | 3D Printed |
| Chairside Time | ~218 minutes per case | ~154 minutes per case | 3D Printed |
| Flexural Strength | Generally higher (80+ MPa) | Comparable or better with 90° orientation | Mixed (PMMA edge) |
| Fit & Accuracy | Good, but shrinkage/distortion possible | Superior dimensional stability | 3D Printed |
| Surface Roughness | Higher | Lower (smoother finish) | 3D Printed |
| Material Cost per Unit | Higher due to waste & labor | 60–70% lower in high-volume workflows | 3D Printed |
| Durability (Long-Term) | Excellent bond & impact strength | ISO-compliant; reprints possible | PMMA edge |
| Patient Comfort | Standard | Improved retention & fewer adjustments |
3D Printed
|
Phase 1: Assessment & Planning (1–2 months)
Phase 2: Technology & Training (2–3 months)
Phase 3: Pilot Cases (Months 4–6)
Phase 4: Full Integration & Scaling (Months 7–12)
Phase 5: Optimization & Leadership (Year 2+)
Clinics adopting this roadmap routinely report 40–60% reduction in total treatment time, higher patient retention, and improved profitability. Retention rates improve, adjustments decrease, and digital records enable lifelong patient management. By 2030, North American practices that remain analog risk losing market share as digital-native competitors dominate.
The transition from heat-cured PMMA to 3D printed resin is not about replacing quality—it’s about amplifying it with speed, precision, and scalability. Clinics that act now will lead the next decade of removable prosthetics in North America.

Dry & wet milling for zirconia, PMMA, wax with auto tool changer.
learn more
High-precision 3D scanning, AI calibration, full-arch accuracy.
learn more
40-min full sintering with 57% incisal translucency and 1050 MPa strength.
learn more

40-min cycle for 60 crowns, dual-layer crucible and 200°C/min heating.
learn more
High-speed LCD printer for guides, temporaries, models with 8K resolution.
learn more