AI Integration in Dental Scanning and Design: Applications, Accuracy & Trends 2026
2026-02-09
2026-03-19
Dental press ingots, primarily lithium disilicate-based, remain a trusted choice for creating highly aesthetic, monolithic or layered crowns, veneers, and inlays through the lost-wax heat-pressing technique. Their excellent translucency, natural light transmission, and strong adhesive bonding deliver superior esthetics with clinical survival rates often exceeding 95% at 5–10 years for single-unit restorations. Yet, despite refinements in material science, persistent processing sensitivities and operational hurdles limit efficiency and predictability in many labs.
This article examines current technical limitations in press ingot technology and the everyday frustrations reported by technicians and dentists. Backed by 2024–2025 in-vitro and clinical data, it provides clear insights for better material selection and workflow optimization in 2026 and beyond.
Press ingots rely on controlled melting and injection into investment molds at high temperatures (typically 900–950°C), but this process introduces inherent material and technique trade-offs.
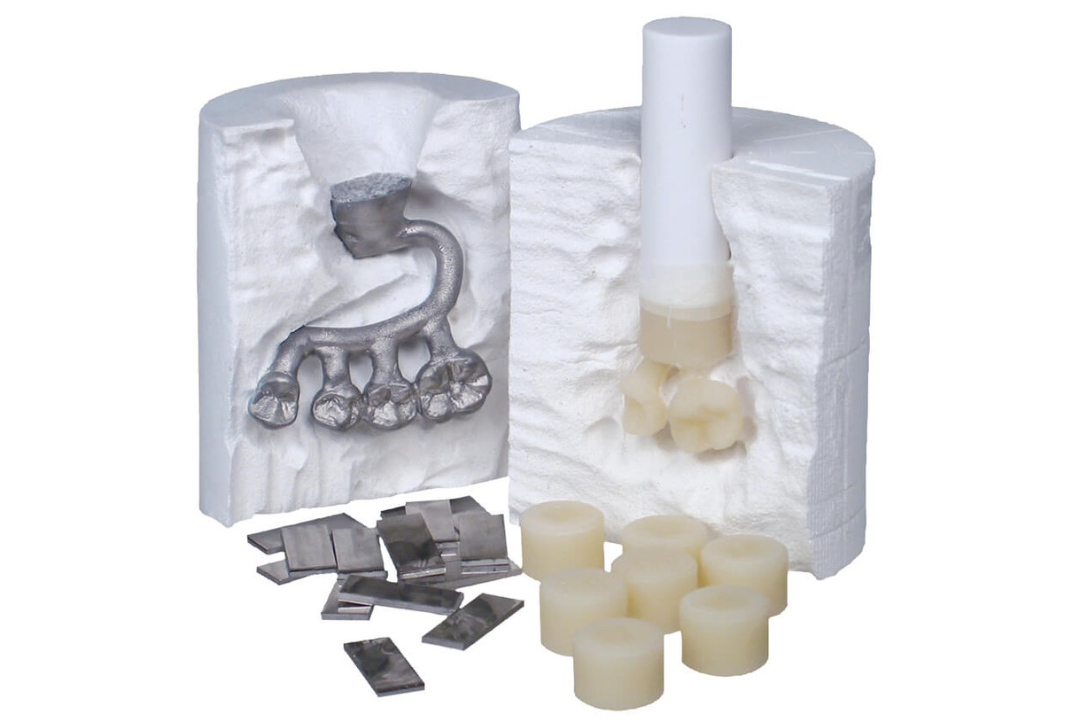
Processing Sensitivity and Microstructural Changes Repeated or improper heat-pressing significantly alters crystal structure. Studies show that multiple press cycles increase crystal size and porosity while decreasing density and flexural strength. One 2024 investigation found that re-pressing lithium disilicate ingots reduced mechanical properties due to larger lithium disilicate crystals and voids. Holding time and exact temperature (even small variations of 10–20°C) critically affect crystallization, leading to inconsistent strength across batches. These sensitivities demand precise furnace calibration and make standardization challenging.
Shrinkage Mismatch and Fit Issues Pressing involves 0.2–0.3% linear shrinkage that must be precisely compensated by investment expansion. Mismatch causes marginal gaps, internal misfits, or distortion. In-vitro accuracy studies comparing pressed versus milled restorations highlight higher deviation in pressed systems when investment or burnout parameters deviate. Poor fit increases remake rates and chairside adjustment needs.
Fracture Toughness and Strength Limitations While monolithic pressed lithium disilicate offers 360–500 MPa flexural strength, it remains lower than zirconia. Posterior restorations show higher fracture risk under heavy occlusion, with chipping or bulk failure more common in bruxers. 2025 comparative studies confirm pressed ingots perform well in single crowns but lag in multi-unit or high-load scenarios compared to CAD/CAM alternatives.
Reaction Layer and Surface Effects Interaction between the ingot and investment material during pressing can form a reaction layer, affecting marginal integrity and bond strength. Over-pressing or incorrect plunger depth risks ring splitting or incomplete filling, as noted in lab troubleshooting reports.
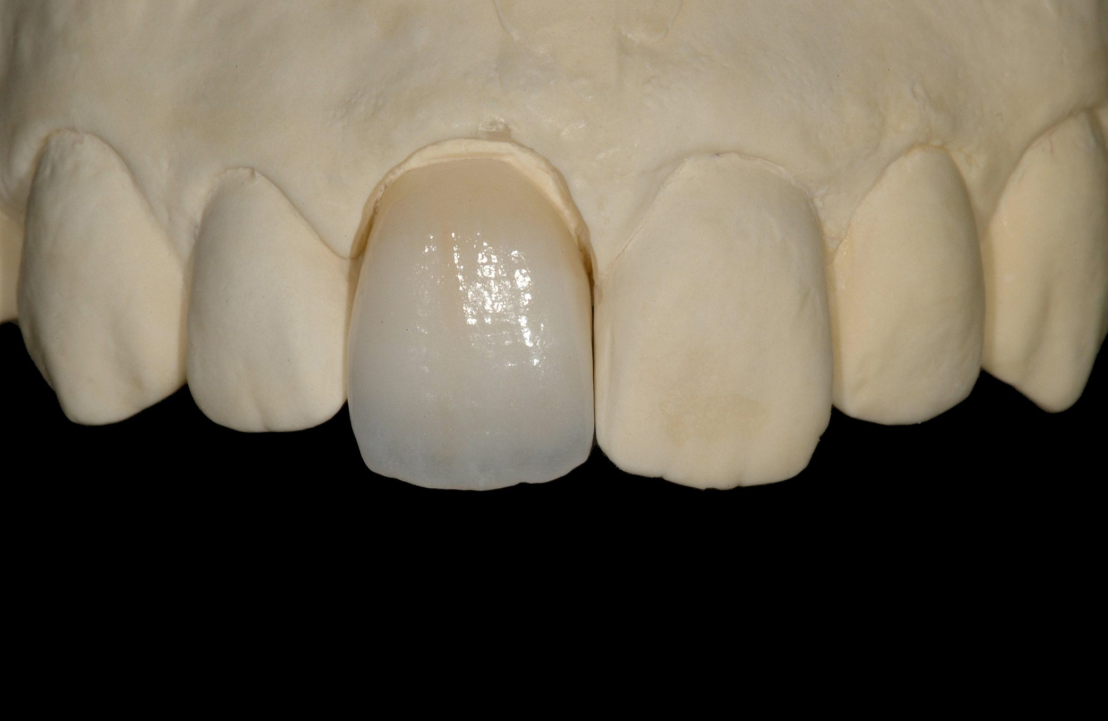
Technicians and clinicians frequently report frustrations that impact lab productivity and restoration longevity.
Time-Consuming Workflow and Turnaround Delays The full process—wax-up, spruing, investing, burnout (hours-long), pressing, and divesting—requires significantly more steps and time than milling. Labs report bottlenecks in high-volume practices, with extended turnaround frustrating dentists and patients. Training new technicians on precise parameters adds further delays.
Technique Sensitivity and Error Risk Small variations in investment mixing, burnout temperature, or pressing cycle lead to defects like porosity, incomplete pressing, or cracks. Users complain about plunger depth issues causing ring fractures and the need for constant furnace maintenance. These errors result in wasted ingots and remakes.
Chipping, Fracture, and Clinical Remakes Even with monolithic designs, occlusal chipping occurs under load, especially if occlusion or polishing is suboptimal. Clinical data show higher non-repairable failure rates in posterior pressed restorations compared to anterior. Adjustments for fit or occlusion introduce microcracks, reducing long-term strength.
Polishing and Aesthetic Challenges Achieving optimal surface finish (Ra <0.2 µm) after pressing and crystallization is labor-intensive. Inadequate polishing leads to staining, plaque retention, or opposing tooth wear. Layered cases require additional veneering steps that introduce thermal mismatch risks.
Equipment and Maintenance Demands Specialized pressing furnaces and investment systems add cost and space requirements. Regular calibration, plunger replacement, and investment quality control increase ongoing expenses and downtime.
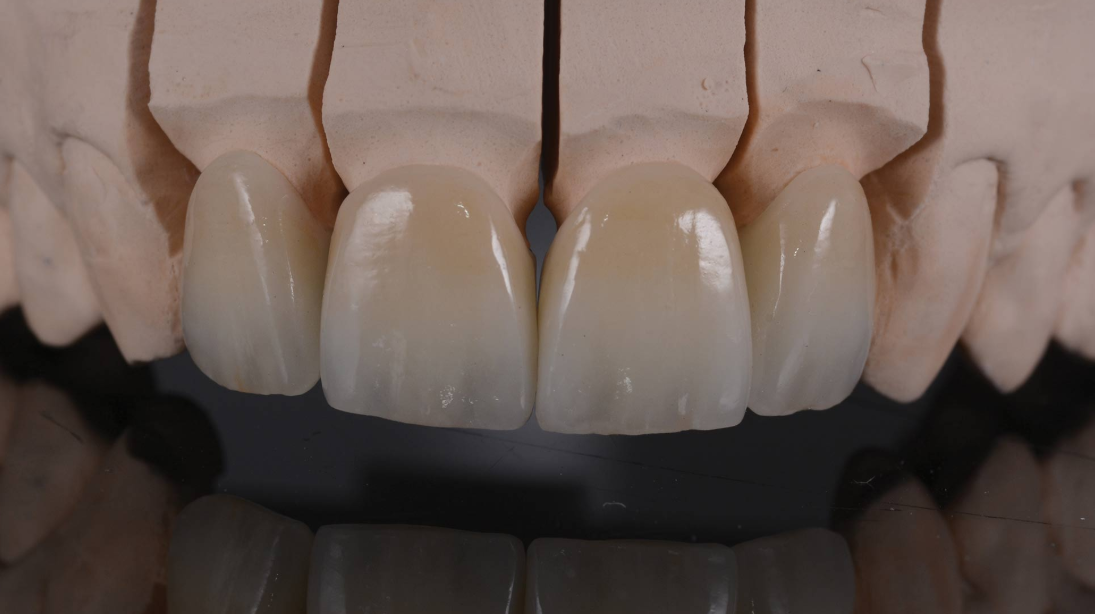
To minimize risks today:
Ongoing advancements—improved ingot formulations with nanostructured fillers, faster crystallization cycles, automated pressing systems, and hybrid press-CAD/CAM workflows—promise reduced sensitivity and faster processing. By 2026–2030, expect wider availability of pre-crystallized press ingots and AI-assisted parameter optimization for more predictable results.
Dental press ingots deliver outstanding esthetics and reliable performance for many restorations, yet processing sensitivity, shrinkage control challenges, strength limitations under load, and workflow complexity continue to challenge labs and clinicians. Technicians consistently demand simpler protocols, more forgiving materials, and faster turnaround without sacrificing quality.
By recognizing these limitations and adopting strict, evidence-based techniques, labs can maximize success rates while reducing remakes and frustration. Press ingots remain a cornerstone of aesthetic dentistry—but precise execution and informed selection are essential for optimal outcomes in 2026 and beyond.

Dry & wet milling for zirconia, PMMA, wax with auto tool changer.
learn more
High-precision 3D scanning, AI calibration, full-arch accuracy.
learn more
40-min full sintering with 57% incisal translucency and 1050 MPa strength.
learn more

40-min cycle for 60 crowns, dual-layer crucible and 200°C/min heating.
learn more
High-speed LCD printer for guides, temporaries, models with 8K resolution.
learn more